Every month a revolutionary discovery?
Every month the specialized press informs us of decisive progress in the treatment of ALS. At the beginning of February, it was a young doctor in Scotland, who turns out to have only done in-vitro experiments showing lengthening of axons of lower motor neurons when subjected to a PGC1α inhibitor, but the press service of his university had translated this as being a great discovery allowing to hope for an ALS drug. It has been known since 2008 that PPAR-γ is a transcription factor that interacts with PGC-1α and that they are involved in ALS.
We are at the end of the month, and here is an important new discovery announcement regarding a treatment for ALS. It is a molecule that has been developed for almost ten years at Northwestern University in Illinois. Several articles have already been written about this molecule. The aim was to find a molecule which is both characterized by low toxicity, capable of crossing the blood-brain barrier and of having an action on the progression of disease. But in 10 years, extensive testing of this molecule had not been carried out on ALS model mice. It would seem that this is the case today, perhaps thanks to the collaboration between two teams, those of Professor Richard B. Silverman who is oriented "chemistry" and that of Professor Hande Ozdinler rather oriented "biology".
There is both good and bad news in this new article. The bad news is that the molecule would only be effective on upper motor neurons. This is a bit surprising and there really isn't any elaborate explanation that would be provided by the authors of the article. Usually in ALS both types of neurons are affected and restoring the functioning of the upper motor neurons will be of little help if the lower motor neurons are unable to control the muscles. In addition, the article is all about restoring the health of diseased neurons, which therefore must treated as soon as symptoms appear.
The authors use very aggressive language
The authors believe that other researchers did not seek to develop therapies for upper motor neurons. This is obviously not true, the number of studies using brain samples from deceased patients are there to testify.
The authors are also not shy about saying that other researchers are enough dumb to do their in-vitro research with different sets of cell lines, sometimes unrelated to motor neuron biology. Since the nervous system involves a lot of different types of cells, and these come from only a few lines of stem cells, on the contrary it seems a very good practice.
In addition, we could counter this focus on neurons by recalling that neurons do not perform their function in isolation, cells collaborate on the same task. Moreover, reading the article one immediately wonders why the authors did not examine the astrocytes, which are only present in the central nervous system.
They further explain that there has never been a study that examines upper motor neurons at the cellular level during the disease. The number of studies on ALS using mice models of the disease is proof of the fallacy of this claim.
A therapy that is effective regardless of the type of proteopathy.
The good news, apparently unexpected, is that the molecule is effective for both SOD1 (about 2% of patients) and TDP-43 (about 95% of patients) pathologies.
In this study, only four thin slices of motor cortex from normal control subjects without neurological disease and nine slices from ALS patients were used in addition to mice studies. Again the number is very low, in other studies several hundred tissues from deceased people are studied. There are also databases that allow data to be shared between researchers.
Histological sections of deceased patients
Upper motor neurons were only counted if their soma and apical dendrite were both visualized in the same 50 µm thick section. This assumes a severe selection of neurons, are the selected neurons representative of the upper motor neuron population?
Identification of NU-9:
The chiral 1,3-Diones cyclohexane, is a cyclohexane molecule containing two ketone groups. As said above, in fact work on NU-9 started almost ten years ago. High throughput screening of over 50,000 molecules was performed using a PC12 cell-based assay expressing SOD1G93A to identify compounds that attenuate protein aggregation and cytotoxicity. This made it possible to identify three families of compounds:
A first compound was selected from over 50 analogues of cyclohexan-1,3-dione, because of its ability to reduce mSOD1-mediated toxicity and inhibit protein aggregation.
Several rounds of optimization were performed, resulting in another compound, which also had excellent pharmaceutical properties in vitro, but did not enter neurons. Further modifications of this compound then led to the generation of NU-9, which crosses the blood-brain barrier, penetrates cortical neurons and has favorable pharmacokinetic properties.
Mouse management
The mice were derived from a cross between SOD1-type ALS model mice and mice carrying a fluorescent protein. In this study, only female mice were used for the experiments. The study involves a very small number of mice, one might wonder if it would be of interest to do a study on such a small number of mice, because no smoothing can erase the inevitable indesirable events. Mice noticeably overreact to tiny variations in their environment, we recently reported that ALS model mice were getting sick at Stanford but not at MIT!
- Ten WT-UeGFP and six hSOD1G93A-UeGFP mice were treated with placebo,
- Five WT-UeGFP mice and seven hSOD1G93A-UeGFP mice were treated with 20 mg / kg / day dose of NU-9.
- Eleven WT-UeGFP mice, nine hSOD1G93A-UeGFP mice and four prpTDP-43A315T-UeGFP mice were treated with a dose of 100 mg / kg / day of NU-9.
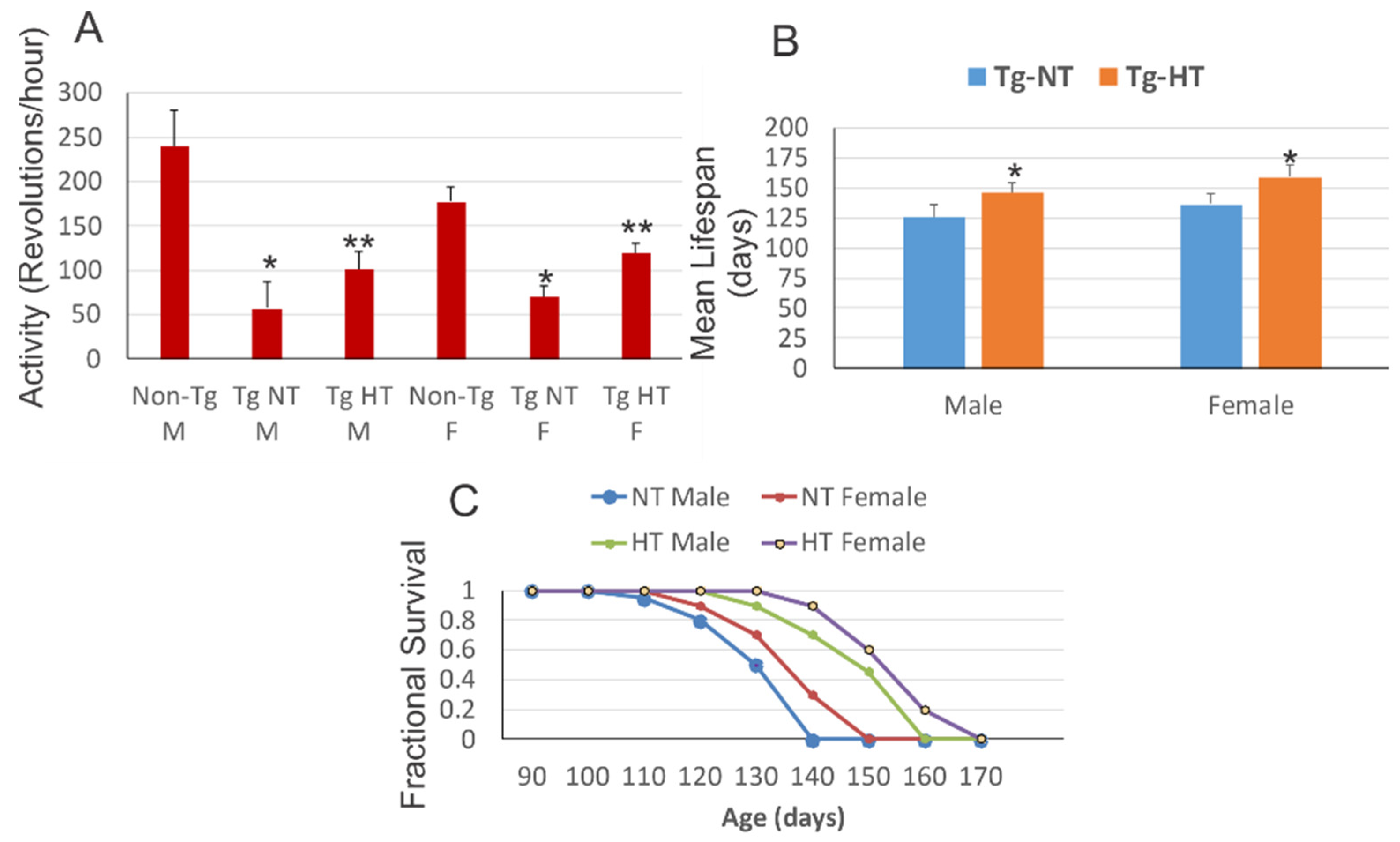
The dose of NU-9 or placebo was administered once daily by oral gavage, starting on postnatal day P60 and continuing until P120. This NU-9 compound is able to prolong the lifespan of an ALS model mouse by 13% with a dose of 20 mg / kg. A repeated 7-day toxicological study in mice demonstrated a no-observed-adverse-effect level of 100 mg / kg.
All of the mice were sacrificed after 120 days (P120), which is considered a terminal stage for this type of ALS model mouse and approximately 60% of the upper motor neurons in the motor cortex are then lost while the motor neurons are lost. remaining upper ones have a smaller soma size and vacuolated and disintegrated apical dendrites. There does not seem to have been any test on an increase in the lifespan of the treated mice.
SOD1 qualitative analyzes
The electron microscope allowed cell type analyzes of upper motor neurons and their key organelles with great precision. At P120, the upper motor neurons of the placebo-treated hSODG93A-UeGFP mice had lost most of their cytoplasmic integrity. There were very few intact organelles left in the soma. However, the presence of disintegrated mitochondria and endoplasmic reticulum was evident. The mitochondria had mostly lost the integrity of their inner membrane, aggregated, enlarged or started to disintegrate. The endoplasmic reticulum also showed broken and scattered cisterns.
NU-9 treatment (dose of 100 mg / kg per day) showed profound improvements in both the structure and integrity of the mitochondria and endoplasmic reticulum of diseased upper motor neurons. Upon treatment, the soma of these neurons showed an intact nuclear membrane, which was devoid of any invagination or protrusion, and the detection of many organelles which were appropriate in size, location and interactions between them. The mitochondrial inner membrane was intact with proper ridges that were in close contact with the endoplasmic reticulum.
SOD1 quantitative analyzes
The authors then performed quantitative analyzes to determine whether these improvements were widely seen in diseased upper motor neurons treated with NU-9. The total number of mitochondria in upper motor neurons of hSODG93A-UeGFP mice was significantly increased after 100 mg / kg / day NU-9 treatment compared to upper motor neurons treated with placebo. The total number of mitochondria after NU-9 treatment was comparable to that of healthy mice. In addition, NU-9 treatment significantly increased the number of healthy mitochondria and endoplasmic reticulum.
present in the motor cortex of hSOD1G93A-UeGFP mice treated for 60 days with 100 mg / kg / day of NU-9 became almost comparable to that of the higher motor neuron numbers present in healthy mice
What about TDP-43?
Since NU-9 appears to improve the integrity of mitochondria and endoplasmic reticulum of upper motor neurons diseased due to mSOD1 toxicity, and these are problems that are also found in pathologies such as TDP-43, the authors speculated that NU-9 might also be effective in TDP-43 pathology. It still seems like a big conceptual step, because they are two distinct disease models. Even if NU-9 has an effect on the structure of the mitochondria and endoplasmic reticulum of higher motor neurons, it should not act on poorly formed and poorly localized protein aggregates that are already present in cytosol? But as the article assumes the drug is administered as soon as symptoms appears, they do not have to deal with that problem.
To test their new hypothesis, the scientists generated a new type of mouse, this time modeling TDP-43 type ALS.
Four mice were treated with a dose of 100 mg / kg / day of NU-9, and 3 mice of the prpTDP-43A315T-UeGFP type were used as a control. The WT-UeGFP mouse cohort was used as a healthy control for both groups.
TDP-43 qualitative analyzes
The NU-9 treatment resulted in profound improvements in both mitochondria and endoplasmic reticulums of higher motor neurons. The mitochondria, especially their internal membranes, became intact and there was no sign of mitoautophagy or mitophagy. The endoplasmic reticulum retained its structure with attached ribosomes, and there was no enlargement or disintegration of the cisterns.
TDP-43 quantitative analyzes
Quantitative analysis confirmed a significant increase in the number of total mitochondria per upper motor neuron per section after 100 mg / kg / day of NU-9 treatment. This number of mitochondria after NU-9 treatment in prpTDP-43A315T-UeGFP mice became comparable to that of healthy mice. The average percentage of healthy mitochondria also increased significantly with NU-9 treatment compared to diseased upper motor neurons. NU-9 treatment also increased the average number of intact endoplasmic reticulum cisterns in upper motor neurons.
The scientists then examined whether NU-9 treatment would also promote cell integrity and the survival of the higher motor neurons with TDP-43 pathology in vivo. The health and integrity of the apical dendrites in prpTDP-43A315T-UeGFP mice showed a profound improvement with the NU-9 treatment because the percentage of upper motor neurons with vacuolated primary apical dendrites was significantly reduced. More interestingly, the mean number of higher motor neurons in the motor cortex of prpTDP-43A315T-UeGFP mice treated with NU-9 was dramatically increased compared to that of untreated prpTDP-43A315T-UeGFP mice.
The same WT-UeGFP cohort was used as a healthy control for the hSOD1G93A-UeGFP and prpTDP-43A315T-UeGFP mice, as mentioned previously. The higher motor neuron numbers with the NU-9 treatment were comparable and almost identical to those of the healthy control mice treated with the placebo, revealing the ability of NU-9 to eliminate the continued degeneration of the higher motor neurons.
Effect of NU-9 on lower motor neurons
In order to determine whether NU-9 treatment also improves the health and survival of lower motor neurons (lower motor neurons), the authors studied the lumbar cords of hSOD1G93A-UeGFP and prpTDP-43A315T-UeGFP mice. As indicated by previous studies, there was no significant loss of lower motor neurons in the spinal cord of prpTDP-43A315T-UeGFP mice, even at P120, and therefore an investigation of NU-9 treatment on motor neuron survival inferior was not possible. This seems to indicate that TDP-43 pathology only affects the higher motor neurons, yet other studies show the opposite.
However, in the case of SOD1, there was a dramatic reduction in the number of lower motor neurons in hSOD1G93A-UeGFP mice compared to healthy mice.
Macroscopic effects
The authors quantitatively assessed the changes in the number of lower motor neurons in the lumbar spinal cord of mice that were treated with either placebo or NU-9 (20 or 100 mg / kg / day), or healthy control mice. . NU-9 treatment, regardless of dose, was not sufficient to eliminate the ongoing lower motor neuron degeneration in hSOD1G93A-UeGFP mice.
NU-9 treatment improves upper motor neuron function Even though most behavioral tests fail to properly assess upper motor neuron health and connectivity, the hanging wire test would be more specific to upper motor neuron integration.
The untreated hSOD1G93A-UeGFP mice could not stay on the hanger as the disease progressed. In contrast, hSOD1G93A-UeGFP mice treated with 100 mg / kg / day of NU-9 performed better than hSOD1G93A-UeGFP mice treated with placebo, and this performance was comparable to that of healthy mice at same age. However, treatment with NU-9 did not result in a significant improvement in performance on the rotarod test at any dose.
The prpTDP-43A315T mice performed worse than the WT litter mates on rotarod and hanging wire tests. However, when treated with 100 mg / kg / day of NU-9, they performed better on the hanging wire test, comparable to healthy WT mice at P120. Unlike the hSOD1G93A mouse model, even the Rotarod test revealed a significant improvement in the TDP-43 model only after 30 days of NU-9 treatment.
Conclusion
The possibility that NU-9 can improve the integrity of both mitochondria and endoplasmic reticulum is important, because, although the underlying causes of the disease are heterogeneous, many clues converge on the proper functioning of the mitochondria and the endoplasmic reticulum. Disruption of intracellular membrane organelles, such as the Golgi apparatus, has been suggested as a possible cause of ALS and is proposed to be upstream of endoplasmic reticulum dysfunction.
This could explain why the NU-9 treatment improves the cytoarchitecture of higher motoneurons and eliminates their progressive degeneration in hSOD1G93A and TDP-43A315T mice.
However, this does not explain why lower motor neurons would not be affected by this molecule. The explanation given that these are different lineages seems very short and has not been further investigated. At no time axons are mentioned in this article, which seems odd in an article that claims to seek a cure for ALS. It seems to me that this weakens the claim that NU-9 treatment improves upper motor neuron cytoarchitecture as this architecture is not extensively tested.
Moreover, the number of mice tested is very, very low and probably statistically meaningless. It is the same for the few histological sections of deceased patients, and the selection of motor neurons. We can also notice that it has been demonstrated for more than 15 years that other types of cells are involved in ALS, starting with astrocytes, than motor neurons. This has absolutely not been studied in this article. However, when a molecule is effective on the higher motor neurons and not on the lower motor neurons, it immediately suggests that it is not on the neurons that it acts, but on the astrocytes!.
All this considerably relativizes the very strong assertions of the press service of the university which reported that "After 60 days of treatment, diseased brain cells look like healthy cells".
For any correspondence write to me at contact [at] padiracinnovation.org


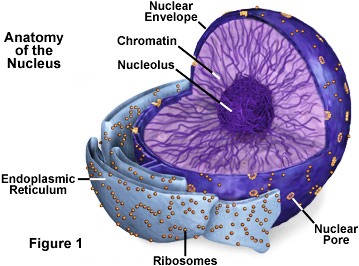
 Source: By Ajpolino via Wikipedia
Source: By Ajpolino via Wikipedia